By Thomas Davis, DNAP, MAE, CRNA
Sometimes the simple things make a big difference in the practice of anesthesia. During the preop assessment, elements of the patient’s social history are noted including smoking, alcohol intake and level of activity. Frequently, “social drinker” is noted but the amount of alcohol consumed is not. In an otherwise healthy patient, an anesthesia provider gives it a quick glance and moves forward with the case.
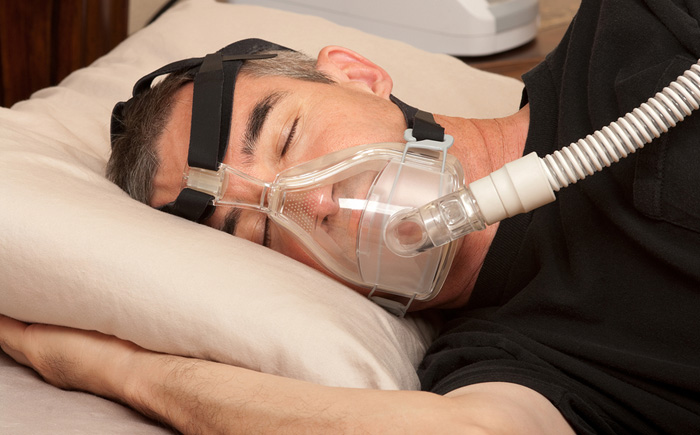
Recently I was made aware of a case in which a male in his late 70’s, normal BMI, otherwise healthy and noted to consume 15 alcohol drinks per week was scheduled for a case using a block and propofol sedation. The block was successfully placed however when the propofol sedation was started, the man exhibited constant movement which continued even as the propofol infusion was increased. Finally, the airway was secured and high dose propofol was infused until the restless movement was calmed. What’s up with that?
An AI review of the literature related to high alcohol intake and paradoxical movement with propofol sedation revealed the following:
- Heavy alcohol drinkers are more likely to experience an excitement response including abnormal movement during propofol sedation.
- Agitation and restlessness are more likely during sedation in patients who drink heavily compared to those who drink little or no alcohol.
- Patients with high alcohol intake are more difficult to achieve optimal sedation with propofol and higher doses of other sedative drugs may be needed.
- Depending upon whether the patient has normal liver function, the onset and duration of sedative drugs may be altered in high alcohol intake patients.
- High alcohol intake may interfere with central nervous system function making it more difficult for the patient to move with coordination and respond predictably.
Both the National Institute for Health and a review published by Florida Anesthesia Services supports the overview listed above and offer suggestions for anesthesia and the high alcohol intake patient.
- Preoperative considerations. Assess and clarify alcohol intake during the preop interview. Ask the patient to define “social drinker” and assume that patients commonly under report their actual alcohol intake. In the case mentioned above, the man who reported 15 drinks per week likely consumed more than admitted. The NIH has an alcohol intake questionnaire that can be used when you suspect that your patient consumes large amounts of alcohol. In addition to clarifying the alcohol intake, assess your patients baseline mobility, nervous system, particularly numbness, and their cognitive function.
- Intraoperative considerations. In the high alcohol patient, higher doses of propofol will likely be required for induction of general anesthesia and hypotension following induction should be anticipated. If a block is planned, consider that the nervous system may be depressed and therefore blocks may last longer than anticipated. When using propofol sedation with a block, anticipate that higher doses may be required to prevent paradoxical movement. If higher doses of sedatives are required, keep in mind the increased risk of postoperative cognitive dysfunction in elderly patients receiving midazolam.
- Postoperative considerations. Heavy drinkers increase the risk of postoperative complications 5 times more than light or nondrinkers. The incidence of delirium, tachycardia, seizures, or a depressed immune system is greatly increased in heavy drinkers. Because we do many of our cases on an outpatient basis it is important to assess the cognitive function of the patient before discharge. In these cases, it is essential to have a reliable person at home to be with the patient immediately after surgery.
In the practice of anesthesia, sometimes the little things make a big difference. After assessing the case of the elderly man with paradoxical movement during propofol sedation followed by a review of the literature, I have a new respect for reviewing the patient’s social history including alcohol consumption. This insight will help me to manage future cases, including a thorough postop evaluation before releasing the patient to go home.
Tom is an experienced leader, educator, author, and requested speaker. Click here for a video introduction to Tom’s talk topics.